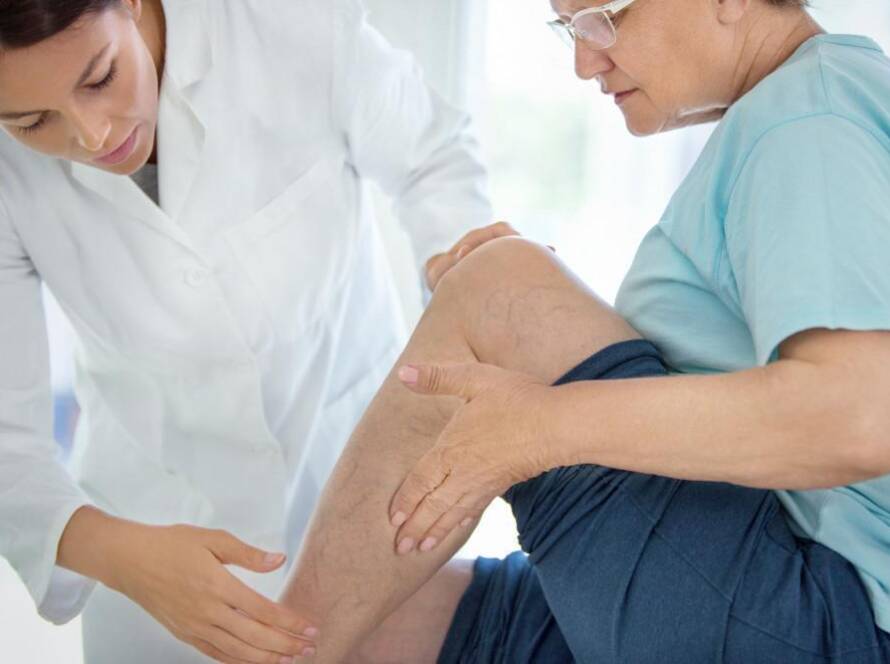
Our team at Premier Vascular in Yonkers and Jackson Heights, New York, led by vascular surgeon Dr. Nirav Patel, provides top-level care for peripheral arterial disease (PAD), varicose veins, chronic wounds, and other conditions related to your circulatory health.
We’re happy to provide information about venous ulcers and what these painful wounds might indicate about your vascular health.
What are venous ulcers?
A venous ulcer is an open sore that typically develops on the inner leg just above the ankle. Most have a reddish base covered by a yellow crust. You may notice skin discoloration, tightness, and warmth in the area before an ulcer develops.
These wounds usually start small and are generally shallow with irregularly shaped borders. However, an ulcer can grow quite large if not treated, sometimes covering significant portions of the lower leg. In addition, a venous ulcer may frequently ooze blood or other material that can indicate an infection.
Venous ulcers can cause significant disability related to lower extremity swelling, pain, persistent skin infection, and tissue death (gangrene) that may eventually require amputation.
What causes venous ulcers?
Venous ulcers are related to poor blood flow through veins in your legs. Veins are the vessels that carry blood back to the heart. Normally, tiny valves in leg veins help keep blood moving upward.
When these valves malfunction, blood pools in the vein and increases pressure in the blood vessel. This causes fluid buildup in nearby tissues and leads to skin breakdown that results in venous ulcers.
Conditions that weaken vein valves or otherwise interfere with normal blood flow through your veins include:
Varicose veins
Deep vein thrombosis (blood clot)
Heart failure
Pregnancy
Prolonged sitting or standing
Chronic venous insufficiency
Diabetes
Excess weight
An inactive lifestyle can also affect circulation since leg veins rely on strong calf muscles to help move blood upward against gravity.
How do you treat venous ulcers?
At Premier Vascular, treatment plans for venous ulcers include advanced wound care that may include:
Specialized dressings to enhance wound healing
Surgical wound debridement
Oral or topical antibiotics
Hyperbaric oxygen therapy
Depending on the size of your venous ulcer, chronic wound care may initially require several weekly visits to our office, and treatments can change as necessary to ensure adequate results.
As part of your care, Dr. Patel may also recommend varicose vein treatment, improved diabetes management, or other therapies that address the issue interfering with blood flow in your leg veins.
You may also benefit from increased physical activity, weight loss, compression stockings, and other home care that improves circulation and helps protect vein health.
Schedule an evaluation with us at Premier Vascular today by calling the nearest office or requesting an appointment online.